Menopause & Hormones
"I have seen how confusing and unsettling hormonal changes can feel, especially during perimenopause and menopause, when symptoms often arrive without warning and seem to shift from month to month. Through years of clinical practice supporting women navigating these transitions, I have learned that lasting relief comes from understanding how hormones are produced, metabolised, and cleared — not from chasing trends or suppressing symptoms in isolation. The insights below offer a clear, evidence-based starting point for understanding what is really happening and how to support your body through it."
Menopause is often spoken about as a moment in time — the point at which periods stop and fertility ends. But biologically, menopause is not an event. It is a long hormonal transition that unfolds over years and influences health for decades afterwards.
To understand menopause properly, it must be understood through the lens of hormonal regulation.
Hormones are chemical messengers. They coordinate communication between organs, tissues, and cells, telling the body how to grow, repair, respond to stress, manage energy, regulate mood, and maintain long-term balance. When hormonal signalling changes, the effects are never isolated to one system.
This is why menopause affects far more than reproductive function.
The hallmark of menopause is a decline in ovarian hormone production, particularly oestrogen and progesterone. These hormones are often thought of as “reproductive hormones”, but this framing dramatically understates their importance. Oestrogen receptors are found throughout the body — in the brain, bones, blood vessels, muscles, liver, skin, and immune cells.
As oestrogen levels fluctuate and then decline, the entire physiological landscape changes.
During the perimenopausal years, hormone levels do not simply fall in a smooth, predictable way. They become more erratic. Oestrogen may surge and crash unpredictably, while progesterone often declines earlier and more steadily. This hormonal volatility explains why symptoms such as mood swings, anxiety, sleep disruption, heavy or irregular periods, and changes in energy can appear long before menopause is formally reached.
These symptoms are not psychological. They are neurological and metabolic responses to changing hormonal signals.
One of the most important roles of oestrogen is its interaction with metabolic regulation.
Oestrogen helps maintain insulin sensitivity, supports healthy fat distribution, and influences appetite and energy expenditure. As oestrogen declines, many women notice that blood sugar becomes harder to manage and fat is more likely to be stored centrally, around the abdomen. This shift increases the risk of metabolic disease and cardiovascular problems, even in women who have never previously struggled with weight.
This is why menopause is a critical window for metabolic health.
Bone health is another area profoundly affected by hormonal change.
Bone tissue is constantly remodelled through a balance of breakdown and formation. Oestrogen plays a key role in keeping this process in equilibrium. As oestrogen levels fall, bone resorption accelerates, often outpacing bone formation. This can lead to rapid declines in bone density in the years around menopause, increasing fracture risk later in life.
Importantly, bone loss during this period is not inevitable, but it is highly sensitive to nutritional status, physical activity, and overall metabolic health.
The brain is also deeply influenced by hormonal change.
Oestrogen interacts with neurotransmitter systems, supports cerebral blood flow, and influences mitochondrial function within brain cells. Changes in mood, memory, concentration, and sleep are common during menopause, not because something is “wrong”, but because the brain is adapting to a new hormonal environment.
When this adaptation is poorly supported, symptoms such as anxiety, low mood, brain fog, and sleep disturbance can become persistent and distressing.
Inflammation tends to increase during and after menopause.
Oestrogen has anti-inflammatory effects. As its influence wanes, inflammatory signalling becomes harder to regulate. This helps explain why the risk of inflammatory conditions, joint pain, cardiovascular disease, and neurodegenerative conditions increases after menopause.
The immune system itself also changes with age, and hormonal shifts interact with this process, further shaping long-term disease risk.
The liver plays a central role in hormonal balance during menopause.
As ovarian hormone production declines, the liver becomes increasingly important for hormone metabolism and clearance. Liver health influences circulating hormone levels, cholesterol regulation, and blood sugar control. When liver function is compromised, menopausal symptoms can become more pronounced and metabolic risk increases.
This highlights an important truth.
Menopause does not happen in isolation. It interacts with metabolic health, gut function, inflammation, stress, sleep, and lifestyle patterns built up over decades. The symptoms experienced during menopause often reflect the cumulative state of the system, not just the absence of oestrogen.
Nutrition plays a powerful role in shaping this transition.
Adequate protein supports muscle and bone preservation. Fibre-rich diets support blood sugar control, gut health, and hormone clearance. Fat quality influences inflammation, brain health, and cardiovascular risk. Micronutrients act as cofactors in hormone metabolism, neurotransmitter synthesis, and tissue repair.
Certain plant compounds, including phytoestrogens found in foods such as soy and flaxseed, can interact modestly with oestrogen receptors and may help ease symptoms for some women. Their effects are subtle, context-dependent, and best understood as part of an overall dietary pattern rather than a targeted intervention.
Healthy ageing through menopause is not about trying to maintain youth or replicate premenopausal hormone levels at all costs.
It is about preserving function.
That means maintaining metabolic flexibility, protecting bone density, supporting brain health, reducing inflammatory load, and sustaining strength and independence as the years pass. Nutrition cannot eliminate menopause, but it can dramatically influence how smoothly the transition unfolds and how resilient the body remains afterwards.
For some women, additional medical support may be appropriate, and nutrition works best alongside informed, individualised care. This is not an either–or conversation. It is about building the strongest possible foundation for long-term health.
The purpose of this page is to give you the full framework for understanding menopause and hormonal change in context. The deeper sections linked below explore specific symptoms, mechanisms, and strategies in more detail.
But everything begins here.
When menopause is understood as a systemic transition rather than a failure or decline, it becomes possible to approach this stage of life with knowledge, confidence, and care — and to lay the foundations for healthy ageing in the decades that follow.
Five Simple Steps For A Healthy Menopause & Beyond
Menopause is not something to “get through” and leave behind. It is a transition that reshapes long-term health. The goal is not to chase youth or eliminate every symptom, but to support the body as it adapts to a new hormonal environment. These five steps help preserve resilience, function, and wellbeing during menopause and in the decades that follow.
1. Prioritise Blood Sugar Stability as Hormonal Support
As oestrogen levels decline, its protective effect on insulin sensitivity is reduced. This means blood sugar becomes harder to regulate, even in women who have never previously struggled with it. Fluctuating blood sugar can worsen fatigue, mood swings, sleep disruption, hot flushes, and central fat gain.
Stabilising blood sugar is therefore one of the most powerful forms of hormonal support during menopause.
Meals built around adequate protein, fibre-rich plant foods, and appropriate fats digest more slowly and place less demand on insulin. Refined carbohydrates and sugars do the opposite, increasing metabolic stress at a time when hormonal buffering is already reduced.
When blood sugar becomes more stable, many menopausal symptoms soften as a downstream effect, because the body is no longer fighting constant metabolic volatility.
2. Protect Muscle and Bone Through Nutrition and Load
Muscle and bone loss accelerate during and after menopause, driven by declining oestrogen, reduced anabolic signalling, and age-related changes in metabolism. This loss has profound consequences for metabolic health, fracture risk, mobility, and long-term independence.
Preserving muscle and bone requires two things: adequate nutritional support and a clear signal that these tissues are still needed.
Protein provides the building blocks for muscle and connective tissue repair, while minerals and micronutrients support bone remodelling. Equally important is mechanical load. Weight-bearing and resistance-based movement stimulate bone formation and help preserve muscle mass.
This is not about intense exercise or aesthetic goals. It is about maintaining strength, stability, and metabolic resilience well into later life.
3. Reduce Inflammatory Load to Support Ageing Systems
As oestrogen declines, its anti-inflammatory influence weakens, and baseline inflammation often rises. This contributes to joint pain, cardiovascular risk, metabolic dysfunction, and cognitive decline after menopause.
Reducing inflammatory load becomes increasingly important.
Diet plays a central role here. Ultra-processed foods, unstable blood sugar, and poor fat quality amplify inflammatory signalling. Whole foods rich in fibre, omega-3 fats, and polyphenols help regulate and resolve inflammation instead.
Reducing inflammation does not mean suppressing the immune system. It means restoring balance, so tissues can repair and regenerate rather than remain in a constant state of low-grade stress.
4. Support the Brain and Nervous System Through the Transition
The brain is one of the organs most sensitive to hormonal change.
Oestrogen influences neurotransmitter balance, cerebral blood flow, sleep regulation, and stress responses. As levels fluctuate and decline, the brain must adapt. When this adaptation is poorly supported, symptoms such as anxiety, low mood, brain fog, and sleep disturbance become more likely.
Supporting the brain during menopause means ensuring steady energy supply, adequate protein and micronutrients for neurotransmitter production, and reducing physiological stress wherever possible.
Sleep deserves particular attention. Poor sleep worsens insulin resistance, increases inflammation, and amplifies emotional reactivity. Even modest improvements in sleep quality can have wide-reaching benefits for menopausal wellbeing.
5. Build Consistency to Support Long-Term Health, Not Short-Term Fixes
Menopause is not a short phase. It is the beginning of a new physiological chapter.
Consistency becomes more important than intensity. Extreme diets, aggressive detoxes, or rigid rules may offer short-term symptom relief, but they often increase long-term stress on the system. The body adapts best to predictable rhythms and reliable support.
Consistent meal patterns, regular movement, adequate rest, and a nutrient-dense diet create an environment the body can trust. Over time, this allows regulatory systems to settle, symptoms to stabilise, and long-term disease risk to fall.
Healthy ageing is not built through perfection. It is built through patterns the body can sustain.
A healthy menopause is not about fighting change. It is about supporting adaptation.
These five steps work because they address the core pressures that menopause places on metabolism, bone, brain, and inflammatory regulation. Applied consistently, they help women move through this transition with greater confidence and emerge into later life with strength, clarity, and resilience.
Everything else builds from here.
Let's Dive Deeper!
Learn More About:

The Key Hormonal Shifts
Understand what actually changes during perimenopause and menopause, why symptoms fluctuate so unpredictably, and how shifting hormones affect the whole body.

Blood Sugar & Weight Gain
Explore how hormonal changes influence insulin sensitivity, fat distribution, and appetite, and why midlife weight gain is more metabolic than willpower.
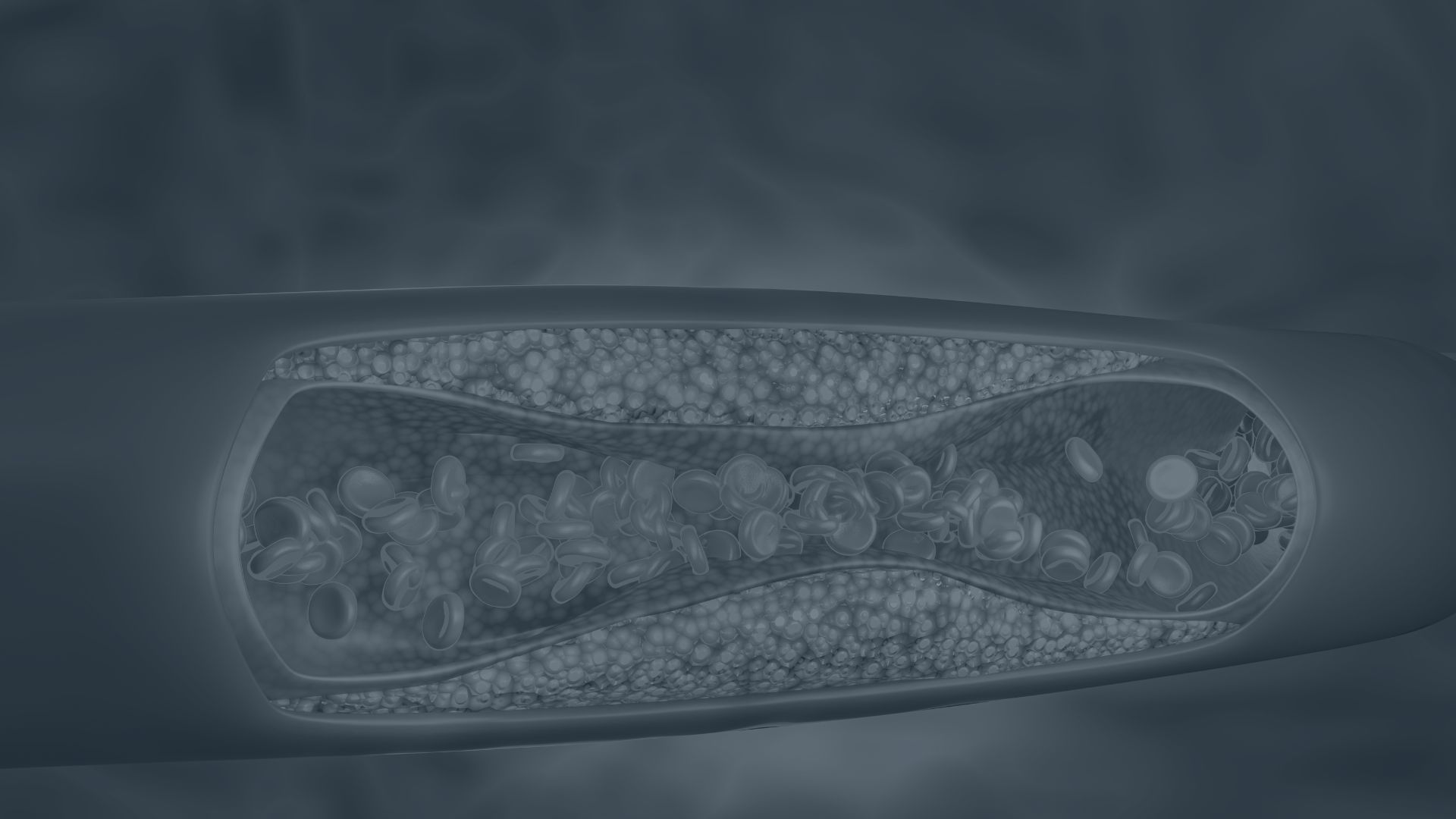
Menopause & Heart Health
Learn why heart disease risk rises after menopause, how oestrogen protects the vascular system, and what lowers inflammation in midlife.

Mood & Mind Changes
Discover how changing hormones affect mood, memory, sleep, and anxiety, and why brain fog is more biological than psychological.
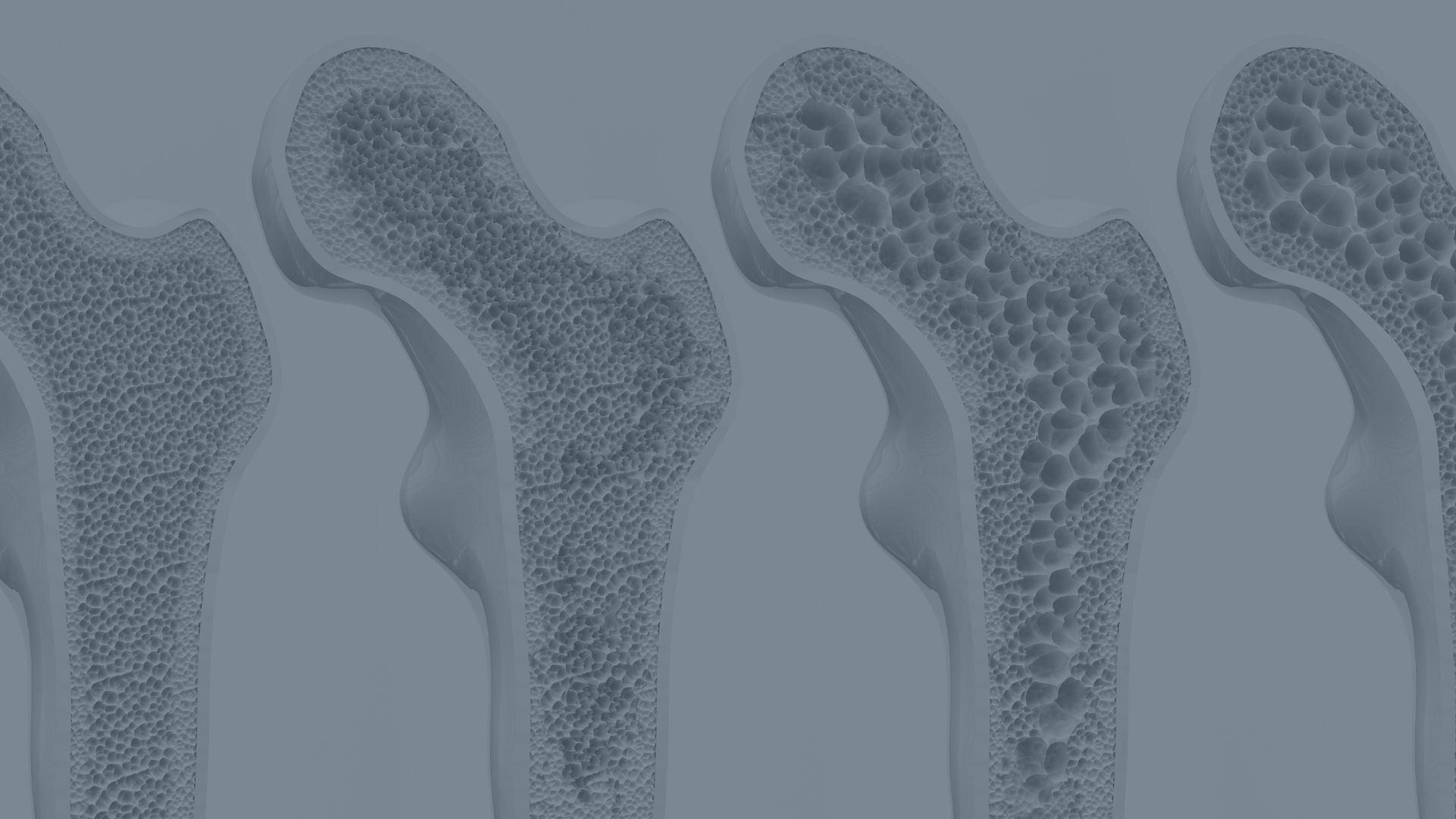
Bone Density & Muscle
Understand how declining oestrogen affects bone strength, muscle mass, and joint stability, and what protects your structure long term.
Sleep Cortisol & Stress
See how menopause reshapes sleep patterns, stress hormones, and nervous system balance, and how to restore calmer, deeper rest.
My Top Recipes For Supporting Menopause & Hormones

Miso Glazed Salmon With Sesame Greens & Soba

Spiced Chickpea, Spinach & Sweet Potato Shakshuka

Warm Lentil, Beetroot & Goats Cheese Salad With Pumpkin Seeds

Tofu, Broccoli & Ginger Stir Fry With Brown Rice

Sardine, Avocado & Watercress Rye Tartines


